Articles > Are You Getting Enough Vitamin D?
Are You Getting Enough Vitamin D?
By Jo /
Vitamin D deficiency is a wide-scale problem affecting many people, not just vegetarians and vegans. It is estimated that more than 50% of people in the UK have insufficient levels of vitamin D and 16% have severe deficiency during winter and spring. So why is this so important?
The consequences of vitamin D deficiency
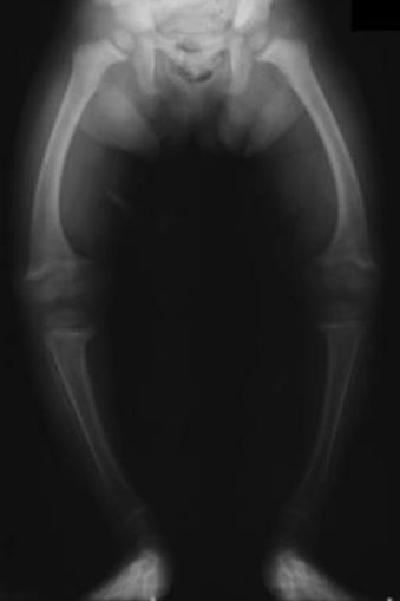
Vitamin D deficiency impairs the absorption of calcium and phosphorus, which affects bone formation. For a long time, it has been known that Vitamin D is necessary for the prevention of rickets in children and osteomalacia in adults. Rickets is a softening of the bones potentially leading to fractures and deformities. It causes bones to be painful and leads to reduced growth. Osteomalacia describes a milder softening of the bones that can occur in adults. This can cause rib, hip, pelvis, thigh and foot pain, and general muscular aches and weakness.
Vitamin D deficiency in pregnant mothers is associated with rickets and an abnormally soft skull in the newborn. Low vitamin D levels (above that associated with rickets in the child) can also adversely affect the child’s skeletal growth, bone and tooth enamel formation. The Committee on Medical Aspects of Food and Nutrition Policy (COMA) recommend that all pregnant and breastfeeding women should consider taking a daily supplement of 10 µg vitamin D in order to ensure their own requirement for vitamin D is met and to build adequate fetal stores for early infancy.
More recently, many other health problems have been found to be associated with low Vitamin D levels, including cardiovascular disease, type I diabetes, several cancers (particularly of the digestive system), cognitive impairment, depression, multiple sclerosis and some other autoimmune conditions.
The current recommended daily intake of Vitamin D in the UK is 400 IU (10 µg) per day for adults, and 280 IU (7 µg) per day for children aged between 6 months and 3 years. However, these recommendations were devised to prevent rickets and osteomalacia, and are now no longer considered to be optimum for good health.
Why might I be deficient in vitamin D?

In a young fair skinned person, 20 to 30 minutes of sunlight exposure on the face and forearms at midday (wearing no sunscreen) two or three times per week, is said to be sufficient to achieve healthy vitamin D levels in summer in the UK. For darker skinned people, and to a lesser extent the elderly, exposure time needs to be increased 2-10 times. These exposure levels can be difficult to attain in our modern world, with so many people working indoors all day. Additionally, from October to April, 90% of the UK lies above the latitude that permits exposure to the UVB wavelengths necessary for vitamin D production, making it impossible for us to make vitamin D during this period. This leaves us dependent upon vitamin D food sources and any vitamin D that has been stored in the body over the summer.

Only a small number of foods contain high amounts of Vitamin D, the most significant being oily fish, cod liver oil and fortified foods such as margarine and breakfast cereals. Foods containing small quantities of vitamin D include egg yolk, wild mushrooms and liver. The amount of vitamin D found in plant foods is negligible. Therefore the typical UK diet is lacking in vitamin D, and this combined with the lack of suitable sunlight, has led to widespread vitamin D deficiency. If you are dark-skinned (of Asian or Afro-Caribbean origin), elderly, pregnant, breastfeeding, obese or wear skin concealing garments, you are at increased risk of vitamin D deficiency. Babies and infants are also at risk, especially those who are breastfed exclusively for more than 6 months, because breast milk is very low in vitamin D.
How can I improve my vitamin D levels?

Many of us are so use to the message to wear sunscreen and cover up whenever we are out in the sun, that we actually forget that the sun provides some benefit to us. Short, regular bouts of midday sun during the summer are useful for raising vitamin D levels. Experts advise spending 20-30 minutes out in the sun two or three times a week, prior to applying sunscreen. However, as mentioned above, this would still not provide enough vitamin D for many people living in the UK, especially from October to April. Additionally, exposure to the midday sun can increase the risk of skin cancer, especially in fair-skinned people. Therefore, supplementation of vitamin D is likely to benefit many of us, especially those who are most at risk of deficiency (outlined in the previous paragraph) or who do not spend much time out in the sun. In the US and a number of other countries, milk is fortified with vitamin D, but in the UK only infant formula and margarine have statutory supplementation.
Which supplements should I use?

The recommended daily dose of vitamin D is 10 µg/day. Supplemental vitamin D is available in two forms, Vitamin D2 (ergocalciferol) and Vitamin D3 (cholecalciferol). Vitamin D2 is synthetically made by exposing a compound from fungus to UV light. Vitamin D3 supplements are produced by exposing a compound from sheep’s wool to UV light. This form of vitamin D is the same as that which is produced in human skin during exposure to the sun. In the past, it was generally thought that the two different forms of vitamin D were equivalent (based on experiments conducted in the 1930’s) however, recent studies have shown that Vitamin D2 is not as potent as Vitamin D3 and it also degrades more rapidly than Vitamin D3.
Vitamin D supplements are available in both forms, however in light of the recent evidence, many companies are now switching from Vitamin D2 to Vitamin D3. As Vitamin D3 is derived from sheep’s wool, vegans may want to use Vitamin D2 instead. Vegetarians and others should preferably choose Vitamin D3 due to the higher efficacy of this type of vitamin D. When choosing supplements make sure you do not take any containing vitamin A if you are pregnant.
Has your vitamin D status ever been measured?
Optimum serum vitamin D concentrations are those above 75 nmol/l, an adequate concentration is 50-75 nmol/l, an insufficient concentration (associated with disease risk) is 25-50 nmol/l and and a deficient concentration (associated with rickets and osteomalacia) is anything below 25 nmol/l. Last year I had a blood test to measure my vitamin D level and I was told that it was 5 nmol/l!
I am young, slim and fair-skinned, I walk about a lot in the sun and I eat a balanced vegetarian diet. So the fact that my vitamin D level was so low came as a big shock to me! It may well be that for some reason my body does not make or absorb vitamin D very efficiently, or perhaps my skin was not getting as much sunlight as I thought. Or maybe I needed to eat more food sources containing vitamin D. In any case, this should be a lesson to others to make sure they are getting enough vitamin D. I am very glad that I went to the doctors and identified the deficiency before it led to anything more serious. I am now on vitamin D supplements for life and I would encourage others in the UK to think more about their vitamin D status, especially those planning pregnancy.
All the scientific facts and figures referred to in this article are taken from the following:
‘Diagnosis and management of vitamin D deficiency’ written by by Professor Simon Pearce and Dr Tim Cheetham published in the British Medical Journal in January 2010.
Scientific Advisory Committee on Nutrition (SACN) ‘Update on Vitamin D’ 2007 report. The SACN is an advisory Committee of independent experts that provides advice to the Food Standards Agency and Department of Health as well as other government agencies and Departments.
‘The case against ergocalciferol (Vitamin D2) as a vitamin supplement’ written by Dr Lisa Houghton and Professor Reinhold Vieth published in the American Journal of Clinical Nutrition in 2006.